ACOG recommends Covid booster shots for pregnant women
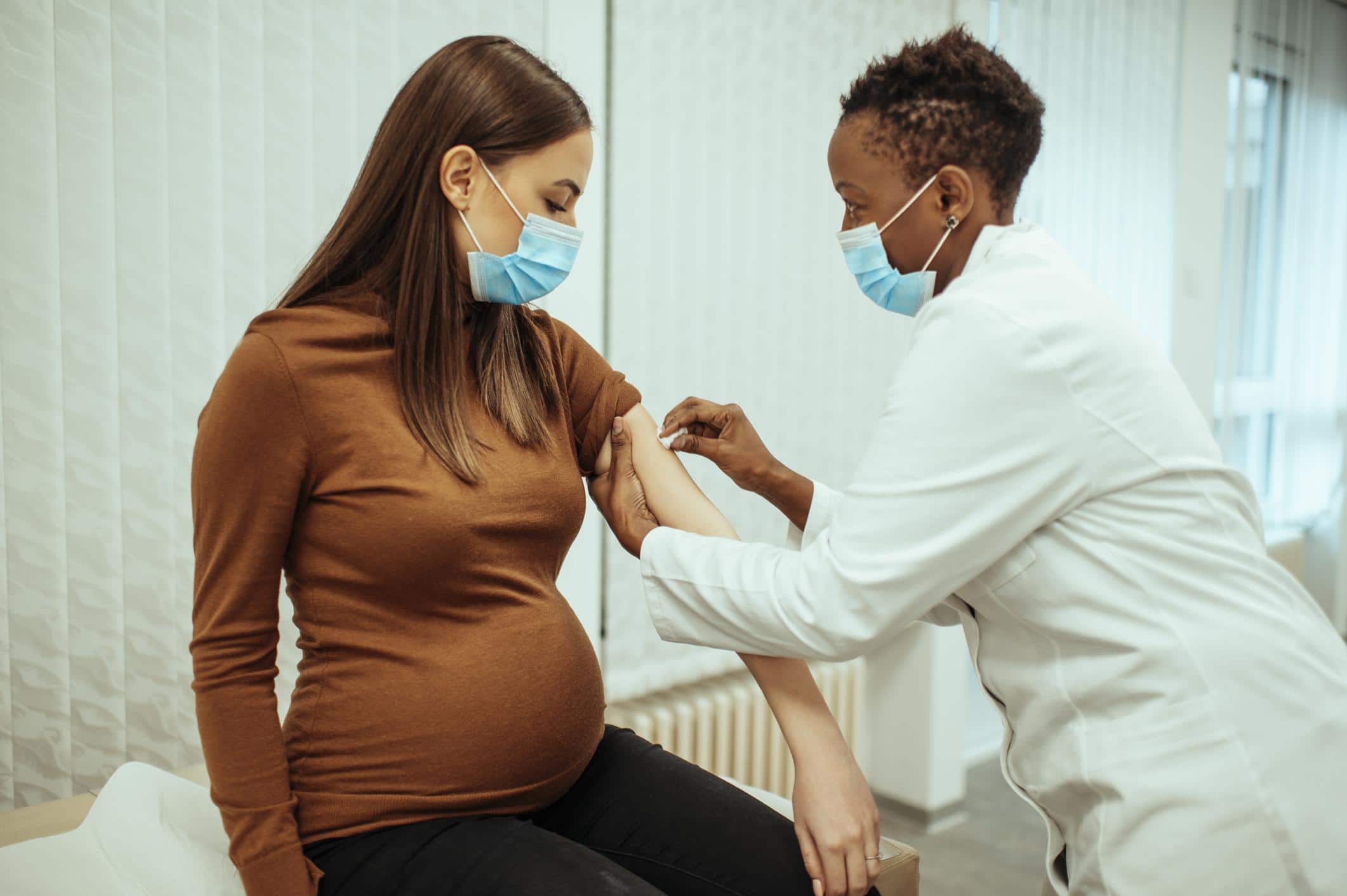
Pregnancy is considered a high-risk state when it comes to severe Covid.
Table of Contents
If you’re pregnant or up to six weeks postpartum and previously vaccinated, the American College of Obstetrics and Gynecologists (ACOG) officially recommends that you get a third dose of the Covid vaccine.
Pregnant people and recently pregnant people were already technically eligible for Covid booster shots of Pfizer or Moderna, as pregnancy is considered a high-risk state and is on the Centers for Disease Control and Prevention’s (CDC) list of health conditions that increase the risk of severe Covid.
Even though the absolute risk of disease is low, if you’re pregnant and contract Covid, you are more than twice as likely to end up in intensive care or require time on a ventilator than a non-pregnant person who has symptoms of the disease. It’s a gamble that’s not worth taking.
Your immune system changes in pregnancy
Because the immune system is naturally weaker during pregnancy, getting sick means your body has fewer defenses to fight off infection—and a virus like SARS-CoV-2 can more easily take hold. Vaccination against Covid is the most effective way to prevent severe disease. And though the vaccines work well even against the highly contagious Delta variant, experts are starting to see slightly waning protection after 6 months from the last dose of an mRNA vaccine, or after 2 months of the J&J/Janssen vaccine.
After a worryingly high number of pregnant women died in August 2021 due to Covid (22), both ACOG and the CDC are still strongly urging pregnant women to get vaccinated if they haven’t yet.
A booster shot offers even further protection, especially if it’s been at least 6 months since your second shot, or you have another underlying condition or work in a high-risk job, like health care or teaching.
“There is a known increased risk of complications from COVID-19 in pregnant patients with underlying health conditions (e.g. diabetes, obesity, increasing age, and cardiovascular disease),” says the CDC.
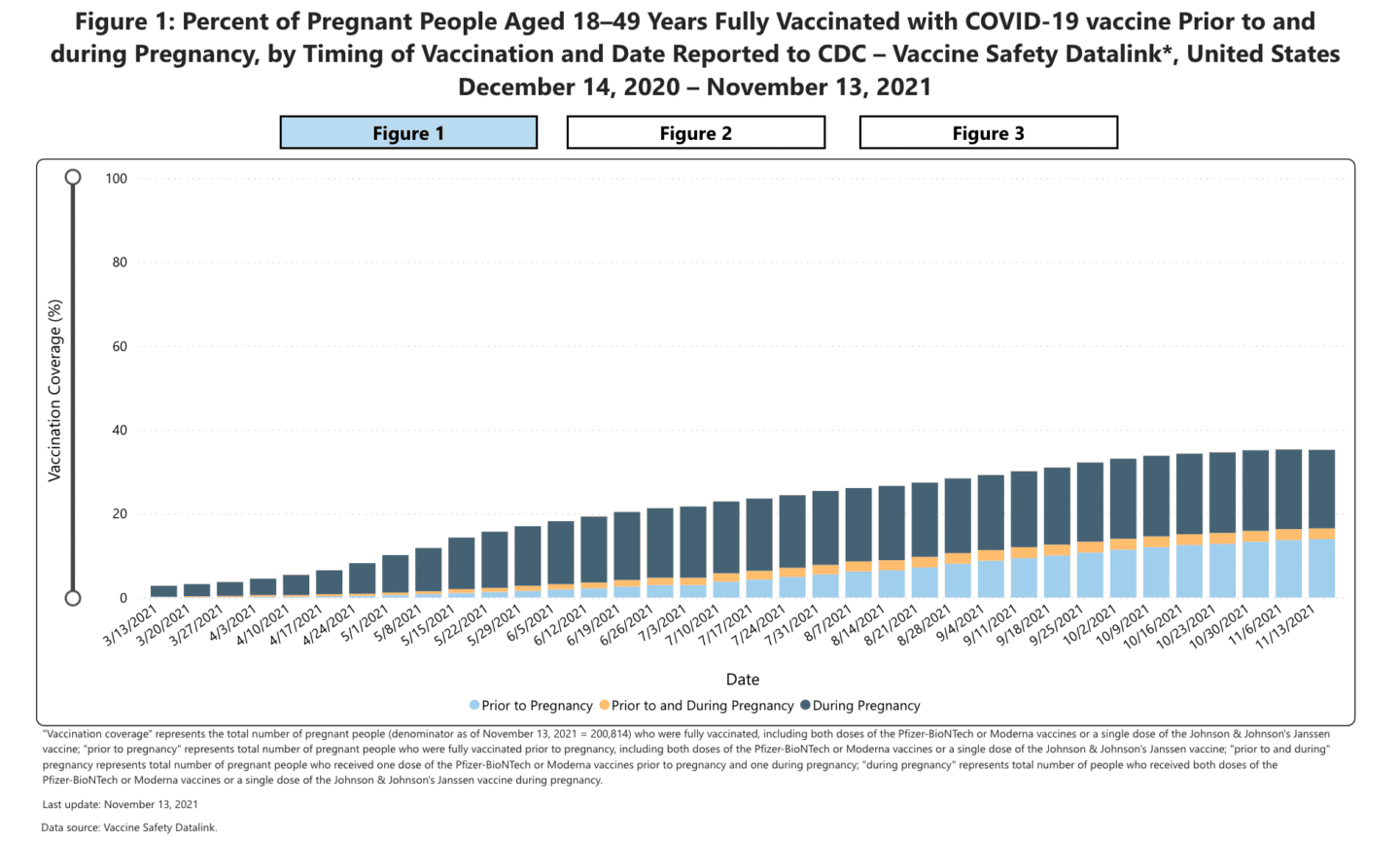
Data indicates that 97% of pregnant people who were infected with Covid when they were hospitalized were not vaccinated—and as of mid-November, just 35.2% of pregnant people in the U.S. were vaccinated, up from 31% in mid-September.
A booster shot now could offer protection to your infant once born
“Pregnancy can be both a special time and also a stressful time, and pregnancy during a pandemic is an added concern for family,” says Dr. Rochelle Walensky, director of the CDC. Talk to your doctor about the benefits of vaccination and any potential risks you’re worried about.
Getting vaccinated in pregnancy can offer significant benefits to your baby:
- A growing body of research shows that antibodies from the vaccine are passed to the fetus when a mother gets vaccinated in pregnancy.
- Because no vaccines are currently available for young infants (under 6 months of age)—and likely won’t be—getting vaccinated yourself is the best way to protect your newborn.
- Even after pregnancy, studies have shown that vaccine antibodies can pass through your breast milk after vaccination.
How to get a Covid booster shot
Your first step should be to talk to your obstetric care provider. Then:
- Call your local pharmacy to see if scheduling an appointment is necessary.
- Be sure to bring your vaccine card.
- You won’t need to provide proof of your pregnancy or underlying medical condition.
Should you mix and match brands of Covid vaccine shots?
You can “mix or match” vaccines should you choose to do so. ACOG and other experts say there’s no risk—and possibly some benefit—to doing so. You can also get your Covid shot at the same time as your flu shot or Tdap vaccine. Be sure to check in with your doctor or midwife for the latest updates.
A version of this post was originally published on Sept. 30, 2021. It has been updated.





































