After 3 years of trying and a round of IVF, I am finally pregnant
It was as if I lived in a world of successive failure. Month after month, benchmarked by my inability to get pregnant. I would break down at every pregnancy announcement.
“Your chances are about 5-7%,” the doctor said flatly. After meeting with two infertility specialists, I found out about my slim chances of a biological pregnancy with IVF.
John, my husband, and I had been trying to conceive for nearly three years. We had baby names picked out before our honeymoon. During the first year of trying, doctors told us to “just be patient, you’ll be pregnant by Christmas.” Well, Christmas came and went and I wasn’t pregnant.
I tracked my ovulation, basal temperature, took Pregnitude, ate royal jelly, and any other possible recommendation, but still never saw a positive pregnancy test. We bought a four-bedroom house in faith that we would eventually have children running around. Friends announced their third, fourth, and fifth pregnancies. We decided to take a trip to Europe.
It was as if I lived in a world of successive failure. Month after month, benchmarked by my inability to get pregnant. I would break down at every pregnancy announcement .
While I was happy that they were able to start a family, it always felt like a reminder of what I wasn’t able to do. John would comfort me every time and listen to my irrational rants, usually cueing up a favorite movie to take my mind off of the hurt.
I switched to a new OB/GYN who recommended a rapid fertility screening, before potentially prescribing Clomid to help us conceive. My husband and I went together for the full screening. Two days later, the doctor called me with the results. My AMH level was alarmingly low.
AMH levels are detected with a blood test and represent a woman’s ovarian reserve or how many eggs are available. This is rarely tested outside of fertility screenings. A normal AMH level ranges from two to seven. Mine was 0.17.
“I’m so sorry,” he said repeatedly.
The doctor wanted to run additional tests on my thyroid because he believed that could explain the low AMH. I immediately went for a blood test that would identify my thyroid levels. Sure enough, I had hypothyroidism in addition to antibodies that resulted in the autoimmune disease, Hashimotos. According to his theory, my thyroid had been attacking my ovaries, resulting in the low ovarian reserve.
At this point, the doctor said that IVF was the only fertility treatment available for our situation. They said that my ovarian reserve was so low, that I was basically running against the clock, at 31 years old.
We spent the weekend absorbing the shock of our new reality.
While the doctor recommended starting treatment as soon as possible, I needed a month of hormone therapy to jumpstart the process. For the next 30 days, I was sneaking away to the bathroom at work to apply testosterone gel to my upper arms and taking estrogen and progesterone pills to help boost my hormones. Ovaries produce hormones and since I had a diminished reserve of ovaries, all of my hormone levels were extremely low.
Thankfully, my body responded appropriately to the hormone therapy and I was cleared to begin a cycle of IVF .
On my 32nd birthday, a large box of injections arrived with my name on them. We unloaded the mini-pharmacy into our bathroom and waited for the instructions we would receive at the next doctor’s appointment.
I was put on the maximum amount of stimulation medications and my husband became my at-home doctor. The concept of IVF is so different from the reality of IVF. There are at least three shots a day, doctor’s appointments almost daily, accompanied by an emotional roller coaster of potentially starting a family, or closing that chapter completely.
“If your body doesn’t respond after a few days, we will cancel the cycle,” said the IVF nurse.
So all of this preparation could literally mean nothing, but we had to try. My husband reached out to friends and family to pray for us because it truly felt like we needed a miracle.
After nine days of stimulation injections, there were eight follicles with potential eggs at a preferred size, so I was cleared for the egg retrieval surgery. And for the first time in three years, we heard positive news from the doctor, saying he was “cautiously optimistic.”
They were able to retrieve seven eggs, but of those seven eggs, only two fertilized. Overnight, our chances dropped to two. It was hard not to feel devastated, however, five days later the embryologist called me to let us know that both embryos made it to a 5-day blastocyst. So our two little embryos were now frozen and ready for transfer.
It is counterintuitive to work tirelessly toward something in such an all-consuming way and then, when it comes to fruition, put it on ice. Frozen embryo transfers have a higher success rate, so we went with our doctor’s recommendation, but it was strange to drive by a hospital and think about our two potential babies frozen in there.
There was another month of preparation, and then, finally, I was ready for the transfer. I elected to transfer both embryos and followed every IVF superstition. I ate pineapple core leading up to and following the transfer, wore socks 24/7 (not an easy feat in the middle of a Texas summer), drank electrolyte water, ate French fries immediately after the procedure and stayed in bed for nearly two days.
Exactly two weeks later, I went into the doctor’s office to take an hCG blood test. When called later with the results, I found out. I was pregnant! I remember thinking that it was all so surreal.
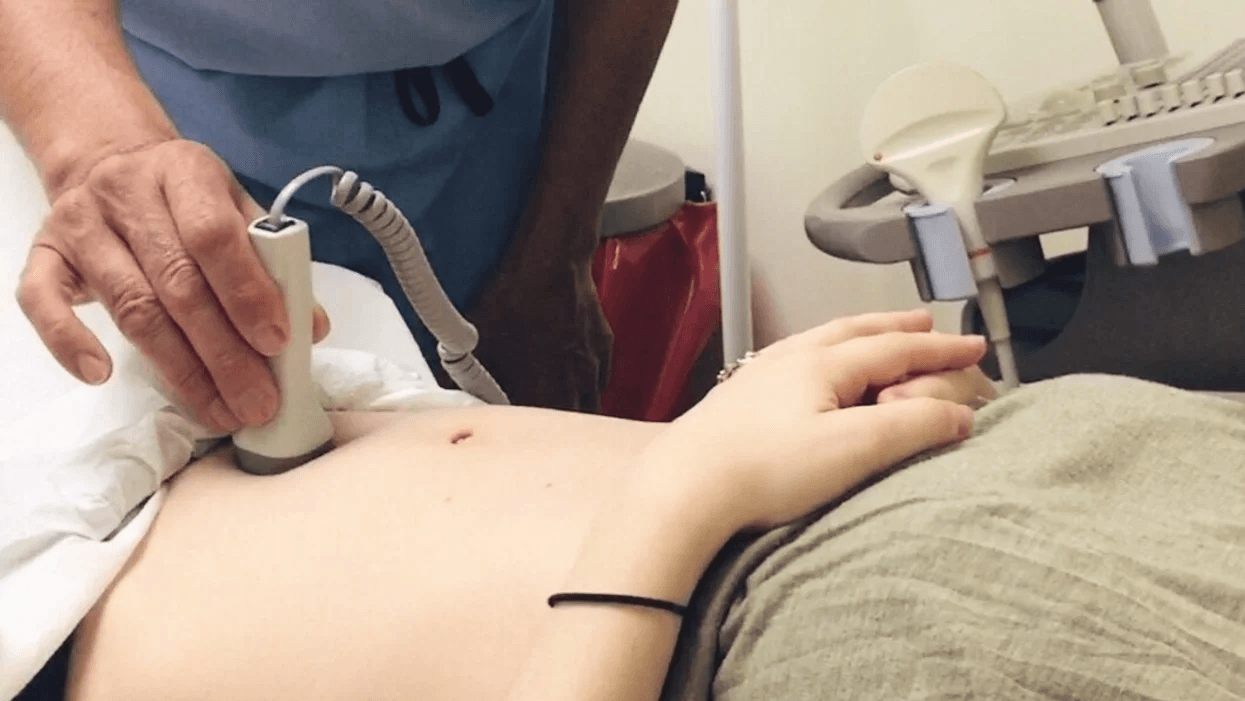
We waited another two weeks to go in for a sonogram that captured the heartbeat, and then, two weeks after that—we transferred from the infertility specialist to a regular OB/GYN. I was (finally!) officially eight weeks pregnant and couldn’t have been happier.





































